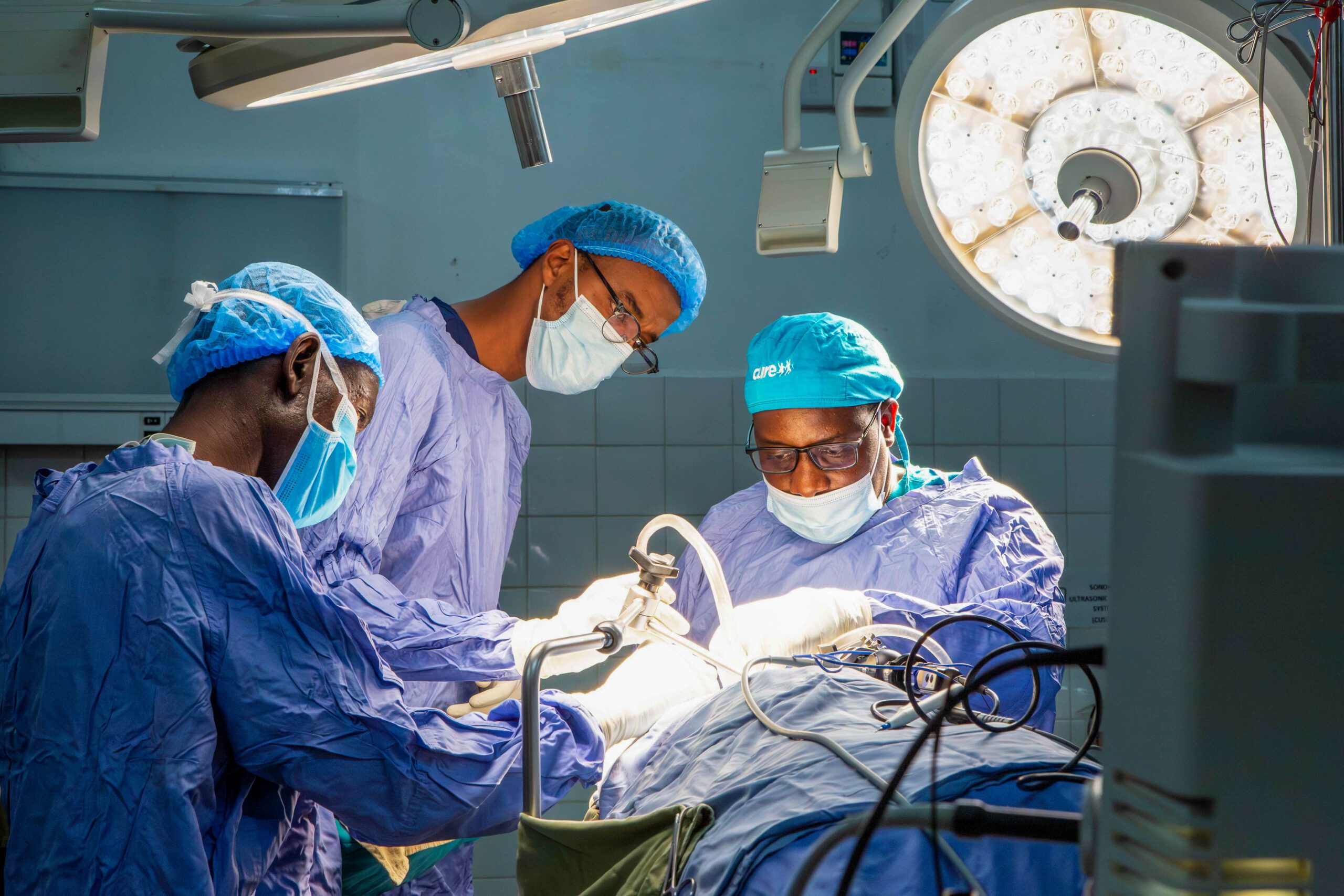
CURE Children’s Hospital of Uganda has become a center of excellence for treating hydrocephalus—a life-threatening condition that affects thousands of babies across the country each year. At the heart of this work is a remarkable surgical innovation called Endoscopic Third Ventriculostomy with Choroid Plexus Cauterization, or simply ETV/CPC. Developed and refined right here in Uganda, it has changed how doctors around the world treat this condition.
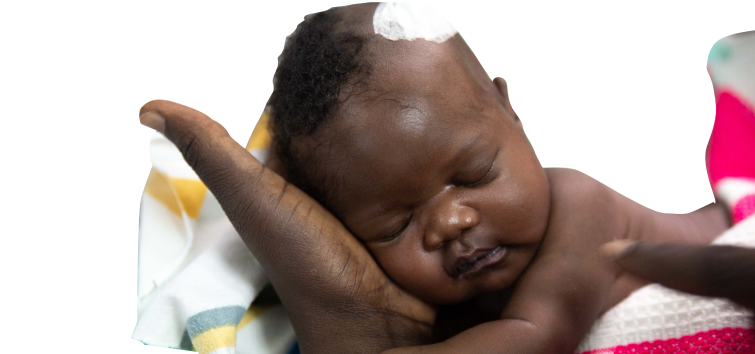
Hydrocephalus happens when cerebrospinal fluid (CSF)—the clear liquid that cushions the brain and spinal cord — builds up inside the brain’s cavities. As the pressure increases, a baby’s head enlarges, and the growing force can damage the brain. If left untreated, hydrocephalus can lead to severe disability or even death.
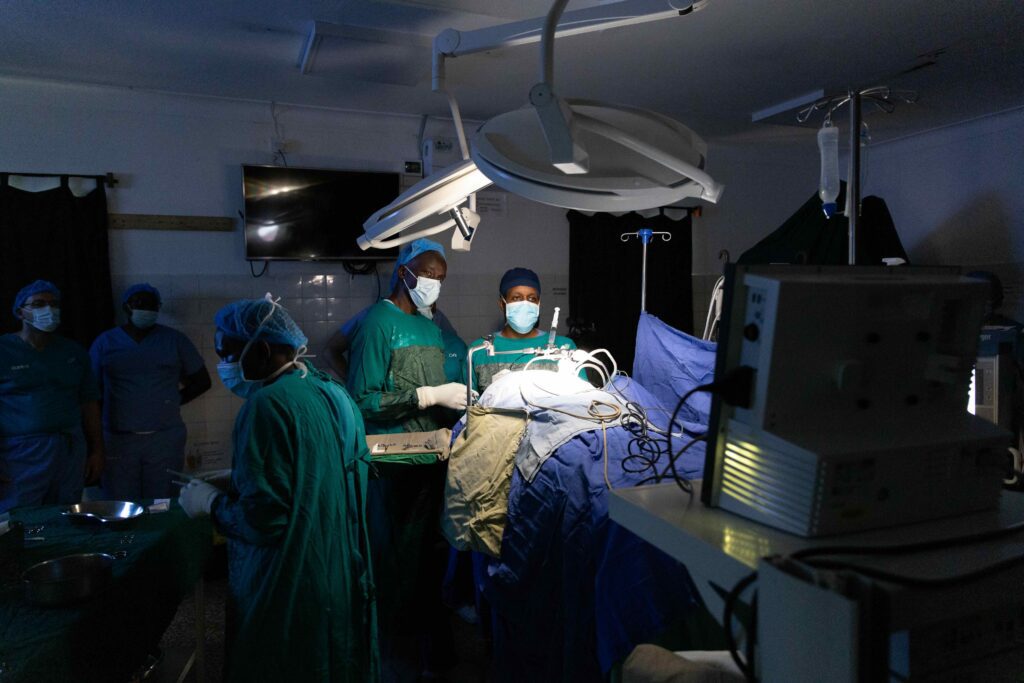
In Uganda, most cases occur after infections in early infancy, such as meningitis or sepsis. This type, known as post-infectious hydrocephalus, is common in low-resource settings where newborn infections are frequent and medical care is limited. It affects thousands of children each year, most of whom are born healthy but later fall ill in their first months of life.
Traditionally, hydrocephalus has been treated using a plastic tube called a shunt, which drains excess fluid from the brain into the abdomen. While effective, shunts fail sometimes, can become infected, or blocked, especially in areas where hospitals are far away and replacement surgery is difficult to access.
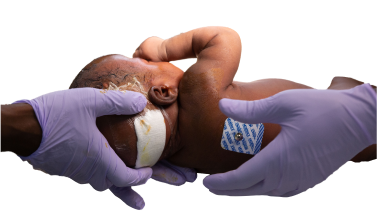
The ETV/CPC procedure offers a better option for many children. In an ETV, a neurosurgeon uses a tiny camera to create a new pathway for fluid to flow within the brain, bypassing the blockage that causes the pressure buildup. The CPC part of the procedure involves cauterizing (lightly burning) part of the tissue that produces the fluid, helping to slow down its formation.
By combining these two techniques, surgeons can often free a child from dependence on a shunt and in many cases, a single surgery is enough to save a child’s life.
Over the past two decades, this approach has been carefully refined at CURE Children’s Hospital of Uganda, guided by both clinical outcomes and the realities of caring for children in low-resource settings. As Dr. Emmanuel Wegoye explains:
“Over the past two decades, the team at CURE Uganda has refined and individualized care for children with hydrocephalus, particularly through the appropriate use of ETV/CPC in our patient population. Our goal is not only to treat these children, but to equip the next generation of neurosurgeons, through the CURE Neuro program, to confidently and appropriately deploy both ETV/CPC and shunt surgeries.”
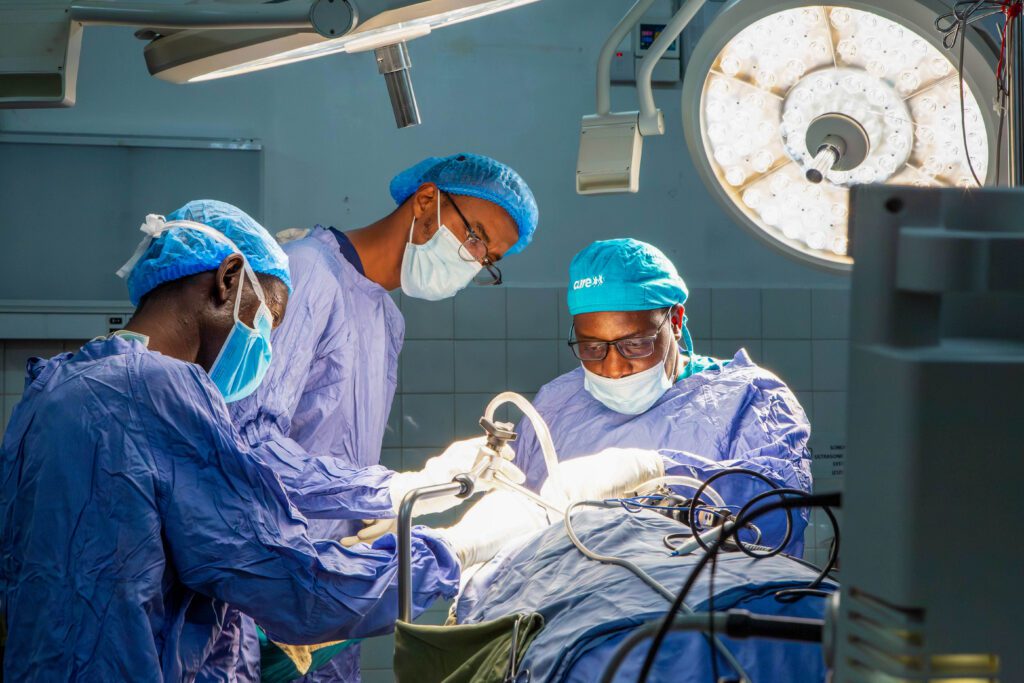
What makes this story even more inspiring is that ETV/CPC was pioneered at CURE Uganda. Under the leadership of neurosurgeons like Dr. Benjamin Warf and the dedicated CURE team, the hospital became the first in the world to routinely perform and perfect this combined procedure in infants.
Today, hospitals all over the world are using this Ugandan-born technique. It has not only transformed local care but also positioned Uganda as a leader in pediatric neurosurgery research and training.
Each year, CURE Uganda treats thousands of children, many from families who could never afford such advanced surgery elsewhere. The hospital’s model of compassionate, faith-driven care ensures that no child is turned away because of cost.
Research from CURE Uganda has shown that ETV/CPC can successfully treat hydrocephalus in many infants who would otherwise require lifelong shunt care. Success rates vary depending on the child’s age and the cause of the condition, but for many, it means freedom from repeated hospital visits, infections, and expensive replacements.
Older infants, and those whose hydrocephalus results from blockages rather than infection, tend to have the best outcomes. Still, even for babies affected by post-infectious hydrocephalus, ETV/CPC offers a safer, more sustainable path than traditional shunting.
For parents, early recognition is vital. A child whose head is growing unusually fast, whose soft spot on the head bulges, or whose eyes appear to gaze downward may have hydrocephalus. Other warning signs include vomiting, irritability, poor feeding, or seizures.
If you notice these symptoms, it’s crucial to seek help quickly from a hospital with neurosurgical services such as CURE Uganda. Early treatment gives the best chance for recovery and healthy development.
Parents should also understand that surgery is only the beginning of the healing journey. Regular follow-up visits allow doctors to monitor progress, ensure the child is developing well, and respond promptly to any complications.
Because many cases stem from infection, prevention also plays a key role. Safe delivery practices, prompt treatment of newborn infections, and proper hygiene during childbirth can all reduce the risk of hydrocephalus developing later
Building Capacity and Spreading Hope
Beyond performing surgeries, CURE Uganda has become a regional hub for training neurosurgeons from across the world. The hospital’s CURE Neuro education programs ensure that more countries can adopt and sustain life-saving treatments like ETV/CPC.
Every day, families arrive at the gates of CURE with fear and uncertainty. Many travel long distances, carrying their children in their arms, praying for a miracle. And every day, stories of transformation unfold, children once given little chance of survival now running, laughing, and attending school.
Hydrocephalus remains a major challenge in Uganda, but progress is being made. Through CURE Uganda’s pioneering work, thousands of children have received a second chance at life. The success of the ETV/CPC procedure has proven that world-class medical innovation can emerge from Africa and save lives far beyond its borders.
For Ugandan families, the message is simple and hopeful: hydrocephalus is treatable. Help is available. And thanks to the skill and compassion of CURE Uganda’s medical team, every child’s story can move from fear to healing, from despair to hope.
If you are a neurosurgeon, pediatric anaesthesiologist, or neurosurgical trainee, this is an invitation to go deeper. At CURE Uganda, the ETV/CPC procedure was pioneered, refined, and proven in some of the world’s most challenging clinical settings, and today that knowledge is being shared with the world. By learning from CURE Uganda’s experience through training, research collaboration, and clinical exposure, professionals can gain practical, evidence-based insight into a less invasive, more sustainable approach to treating hydrocephalus. Join a global community committed to reducing shunt dependence, improving long-term outcomes, and ensuring that life-saving innovation reaches the children who need it most—wherever they are.
About the CURE Children’s Hospital of Uganda
CURE Children’s Hospital of Uganda has been a place of hope since opening its doors in 2001. It is one of Africa’s leading pediatric hospitals for brain surgery and the treatment of neurological conditions. Our teaching hospital has an 18-bed Intensive Care Unit and 59 ward beds, three operating rooms, and an outpatient clinic. In addition to world-class medical care, our team ministers to the emotional and spiritual needs of our patients and their communities.